In a quiet farmhouse in rural Utah, hundreds of miles from the nearest metropolitan center, a pregnant mother wakes up and waits for a fetal movement that does not come. In this region of the United States—identified as one of the many "medical deserts" where approximately 30% of counties lack a single practicing obstetrician-gynecologist—the nearest specialized hospital is often a 500-mile journey across difficult terrain. Historically, this silence from the womb triggers a predictable and harrowing sequence: a desperate phone call to a health maintenance organization (HMO), a checklist of questions from a remote nurse regarding diet and hydration, and an inevitable, high-stress drive to an emergency room that may take half a day to reach.
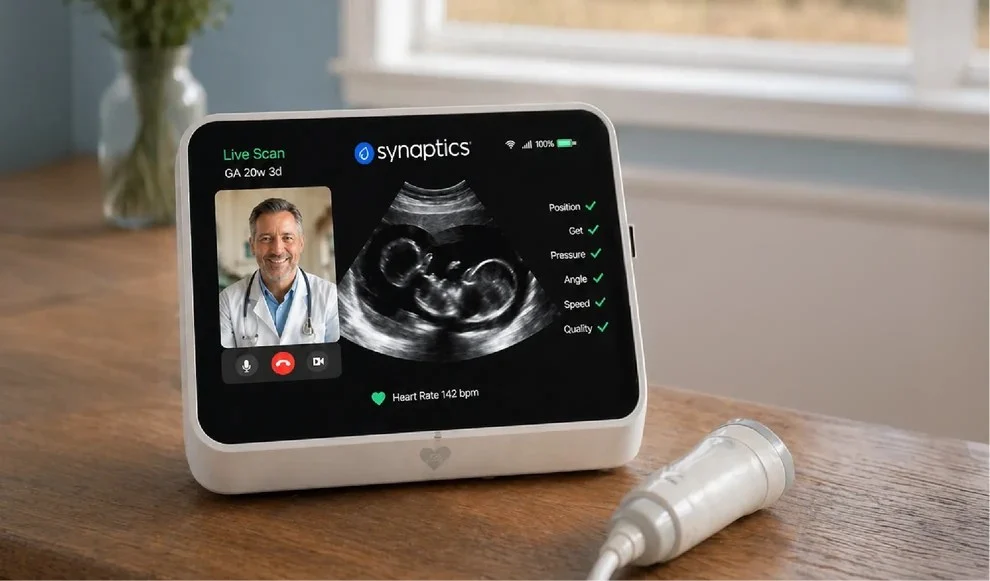
However, a technological shift is altering this narrative. Instead of reaching for her car keys, the mother reaches for a handheld ultrasound cradle. She applies the acoustic gel and begins to glide the probe across her abdomen, guided not by a technician in the room, but by edge artificial intelligence (AI) embedded directly into the hardware. The device provides immediate, audible feedback. When she moves too quickly in her anxiety, the system instructs her to slow down. When she inadvertently positions the probe over her own heart, the system recognizes the latency-free data and warns her that she is capturing her own maternal pulse rather than the baby’s. By forcing precision—requesting more gel or a change in location—the device ensures the resulting scan is clinically usable. Within three minutes, the session is complete. Because the device processes eight to ten critical parameters locally and in real-time, it identifies potential crises without needing a stable cloud connection. The data is then transmitted to a physician who can review the high-quality imagery and dispatch emergency services if necessary.
The Growing Crisis of Maternity Care Deserts
The emergence of home-based diagnostic tools comes at a critical juncture for global healthcare systems. In the United States, the March of Dimes reports that more than 2.2 million women of childbearing age live in maternity care deserts—counties without a hospital or birth center offering obstetric care and without any obstetric providers. Between 2004 and 2014, 9% of rural counties in the U.S. lost their last remaining hospital-based obstetric services, a trend that has only accelerated in the last decade due to staffing shortages and economic pressures on rural healthcare facilities.
For patients in these regions, the standard of care is often compromised by geography. Routine prenatal monitoring, which requires frequent sonograms and check-ups, becomes a logistical and financial impossibility. This disparity leads to higher rates of undetected complications, such as preeclampsia, gestational diabetes, and fetal growth restriction. The transition of medical imaging from the sterile, controlled environment of the clinic into the home is no longer just a convenience; it is a clinical necessity for rural and underserved populations.
Pioneering the Shift to Patient-Operated Hardware
Bridging the gap between a professional sonographer and a layperson requires more than just miniaturizing hardware. Ultrasound technology is notoriously operator-dependent; the quality of the image relies heavily on the "hand that holds the skin." Variations in a patient’s Body Mass Index (BMI), the specific week of gestation, and the pressure applied to the probe can drastically alter the diagnostic value of a scan.
To address this, companies such as Pulsenmore are pioneering a new paradigm where the patient becomes the operator of complex medical hardware. However, moving a sophisticated tool into the hands of an untrained user introduces significant risks to clinical reliability. If a patient captures a sub-optimal image, a physician cannot make an accurate diagnosis, rendering the remote session useless. The integration of edge AI serves as the solution to this problem, providing a "digital coach" that ensures every scan meets the high bar required for medical decision-making.
The Technical Necessity of Edge AI Over Cloud Computing
The primary engineering hurdle in developing home-use medical devices is ensuring data accuracy in real-time. Traditional AI models often rely on cloud-based processing, where data is transmitted to a remote server, analyzed, and sent back to the user. In a medical context, this loop introduces "latency"—a delay of several seconds that can be catastrophic during a diagnostic procedure.
In medical imaging, where a patient is physically moving a probe, those seconds represent a significant gap in feedback. If a patient is scanning the wrong area, a cloud-based alert arriving five seconds later is useless, as the patient has already moved the probe elsewhere. By processing data at the "edge"—directly on the device’s internal silicon—the system provides instantaneous feedback.
Furthermore, high-resolution ultrasound devices generate a massive volume of data, typically around 25 images per second. Processing this entire stream in the cloud is not only slow but prohibitively expensive and bandwidth-intensive, especially in rural areas with poor internet connectivity. By utilizing AI-native embedded compute platforms, such as the Synaptics Astra portfolio, these devices can process critical parameters locally. This ensures that the remote physician receives a curated, high-quality data set rather than a fragmented or low-resolution stream.
Engineering the "Intelligent Handshake"
The collaboration between medical hardware developers and semiconductor innovators like Synaptics focuses on creating an "intelligent handshake" between the machine and the human user. This involves building AI models that monitor environmental factors and user movements simultaneously.
Through a synchronized mobile application, edge AI provides audible and visual alerts to standardize the scanning process. Technical features include:
- Acoustic Coupling Monitoring: Detecting if there is insufficient gel on the abdomen and alerting the user to add more to ensure clear imaging.
- Velocity Tracking: Monitoring the speed of the probe movement and instructing the user to slow down to prevent image blurring.
- Anatomical Recognition: Identifying whether the probe is over the uterus, the bladder, or the maternal heart to ensure the correct organs are being imaged.
This real-time quality control reduces "miss-cases" and errors that can occur even in clinical settings when staff are fatigued or overworked. By the end of a short learning curve, even a first-time user can produce a standardized, reliable medical image.

The Hardware Balancing Act: Cost vs. Performance
Developing reliable edge AI for the consumer medical market requires a delicate balancing act. Dr. Elazar Sonnenschein, CEO of Pulsenmore, describes the engineering challenge as a "blanket with four corners": developers must balance algorithm complexity, memory requirements, processing horsepower, and price.
Unlike hospital equipment, which is a capital investment designed to last for a decade, home medical devices are often intended for a single pregnancy or a specific treatment window. This necessitates a lower price point. To make these devices accessible, engineers must use silicon that provides high performance without the cost of high-end server chips. The use of power-efficient, natively secure processors allows these devices to run complex AI models on battery power while maintaining the data privacy required by healthcare regulations such as HIPAA.
The team at Synaptics worked to match the performance and regulatory needs of Pulsenmore by selecting specific embedded processors that could handle the computational load of ultrasound AI without inflating the retail cost. This ensures the technology can be scaled to millions of households rather than remaining a luxury for the wealthy.
Regulatory Benchmarks and Clinical Validation
For a medical-grade edge AI device to gain widespread adoption, it must move beyond technical functionality and meet rigorous regulatory standards. This involves proving that the AI is consistent, unbiased, and accurate across diverse populations.
The AI models used in these devices are trained on massive, proprietary datasets. For instance, Pulsenmore’s models are informed by hundreds of millions of images from hundreds of thousands of historical scans. This scale allows the AI to recognize rare clinical edge cases and abnormalities, such as a fetal heart rate falling below 100 beats per minute or rising above 160, which may indicate fetal distress.
By demonstrating this reliability through extensive clinical trials, these devices have secured FDA De Novo clearance and international medical certifications. This regulatory approval is essential for integrating home-based scans into the official medical record, allowing doctors to treat the data with the same level of confidence as an in-hospital ultrasound.
Real-World Outcomes: From Data to Life-Saving Intervention
The ultimate objective of edge AI in healthcare is not merely technical efficiency but the preservation of life. The impact of this technology is already being felt in international markets. Dr. Sonnenschein cites a specific case in Israel where an expectant mother used a home ultrasound device during a period of perceived reduced fetal movement.
The AI-guided scan, performed in her living room, revealed that the umbilical cord was wrapped around the baby’s neck—a condition known as a nuchal cord complication. Because the device identified the emergency parameters and transmitted the data instantly to a remote physician, an ambulance was dispatched immediately. The mother underwent a successful emergency C-section within an hour of the scan. Both the mother and her baby girl were saved by the immediacy of the data.
This case highlights the shift from synchronous care (where the doctor and patient must be in the same place at the same time) to asynchronous care. In an asynchronous model, the patient can perform a scan at 2:00 AM, and the AI ensures the data is of sufficient quality for a doctor to review it minutes or hours later from any location in the world.
The Future of Medicine at the Edge
The success of edge AI in maternal health provides a blueprint for the future of decentralized medicine. The principles applied to home ultrasound—real-time guidance, local data processing, and cost-effective hardware—are currently being explored for other diagnostic areas, including cardiac monitoring, chronic kidney disease management, and respiratory health.
As the global healthcare infrastructure continues to face challenges from aging populations and provider shortages, the "hospital at home" movement will rely heavily on the intelligence embedded in consumer devices. The goal is a future where "medical deserts" no longer dictate a patient’s health outcomes.
The technology to eliminate the choice between waiting in fear and driving hundreds of miles for answers is no longer a futuristic concept; it is currently in production. The challenge for the industry moving forward is to scale these solutions responsibly, ensuring that high-quality medical imaging is a right accessible to everyone, regardless of their proximity to an urban hospital. The future of healthcare is moving away from centralized institutions and firmly toward the edge.